Brown & Brown UnitedHealthcare Medical Plans & Express Scripts Prescription Drug Coverage
B&B UnitedHealthcare Medical Plan & Express Scripts Rx Overviews
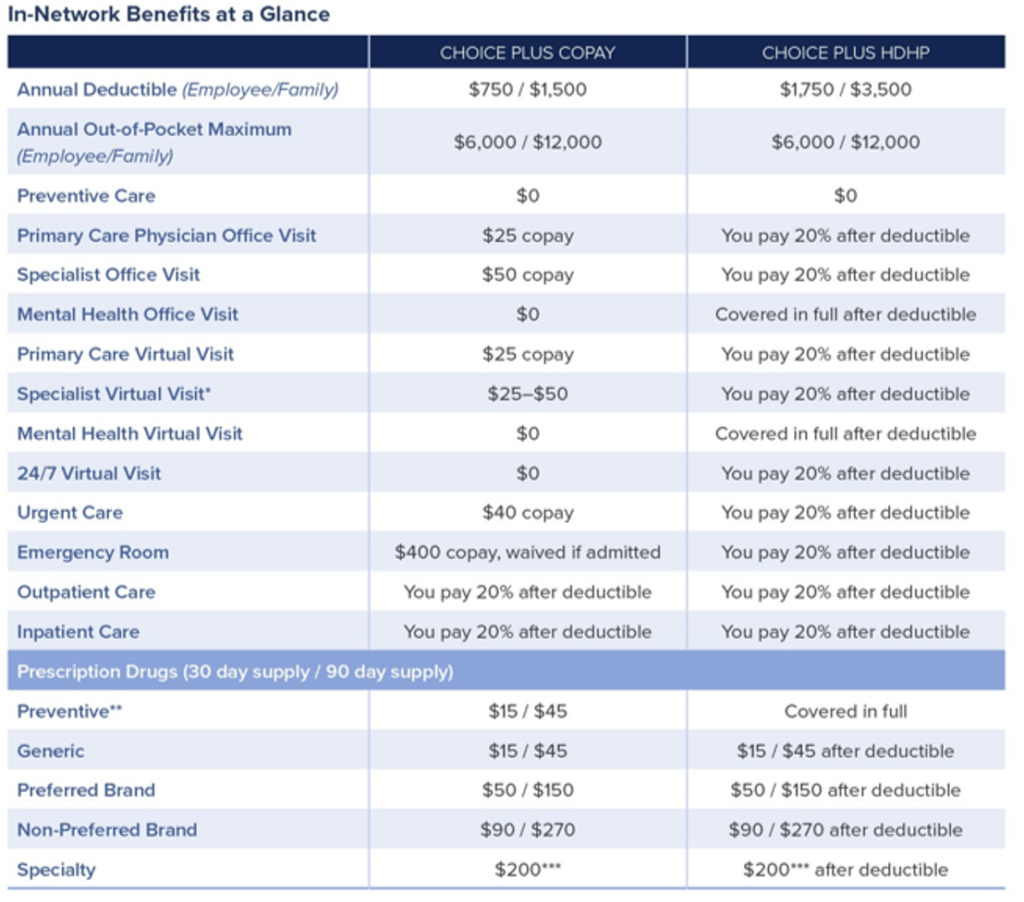
The Brown & Brown, Inc. Self-Funded Healthcare Plan offers two medical plan options with administrative services provided by UnitedHealthcare (UHC) and Optum Bank for the Health Savings Account.
Prescription Drug Benefits for both plans are through Express Scripts, Accredo for Specialty Rx and PillarRx Copay Assistance.
What are my plan options?
Choice Plus Copay Plan
- 2024 Choice Plus Copay Benefit Summary
- 2024 Choice Plus Copay SBC
- 2024 Choice Plus Copay Benefit Summary Harvard Pilgrim
- 2024 Choice Plus Copay SBC Harvard Pilgrim
Choice Plus HDHP/HSA Plan
- 2024 Choice Plus HDHP Benefit Summary
- 2024 Choice Plus HDHP SBC
- 2024 Choice Plus HDHP Benefit Summary Harvard Pilgrim
- 2024 Choice Plus HDHP SBC Harvard Pilgrim
*Teammates in Maine, Massachusetts and New Hampshire will utilize the Harvard Pilgrim Network
Prescription Drug Benefits through Express Scripts, including Accredo for Specialty Pharmacy, and PillarRx Copay Assistance for both plans
- Welcome to Express Scripts Guide
- 2024 Express Scripts Choice Plus HDHP Preventive Drug Listing
- 2024 Express Scripts National Preferred Formulary
- Accredo Specialty Medications FAQs
- Accredo Patient Journey
- PillarRx Copay Assistance Program FAQs
- Weight Loss Medications and Omada FAQs
Important Note About ID Card Distribution: UHC Medical and Express Scripts Rx are combined on one UHC ID card. Hard copies of UHC medical cards will only be issued to teammates who are enrolling in coverage for the first time and for teammates that do not select ‘paperless’ as the required communications. Digital ID cards will be available for teammates who choose ‘paperless’ and can be saved to smart phone wallets to share with providers.
Brown & Brown Health Concierge - Enhanced Advocacy Service
Teammates and eligible dependents enrolled in one of the Choice Plus medical plans administered by UnitedHealthcare (UHC) will have access to an enhanced advocacy service—Brown & Brown Health Concierge—to help navigate the complicated world of health benefits.
This free service provides a dedicated Health Concierge who can guide and assist with understanding and managing claims, finding providers, making medical and behavioral health appointments, securing a second opinion on a medical diagnosis and more.
Call 1-844-298-8929 to connect with a trained health care advocate who can help answer your health care questions and connect you with the best resources available to you. The Health Concierge number is also listed on the back of all UHC medical ID cards.
Additional Benefits Information for Both Plans
Both Medical Plans Include:
Teammates and eligible dependents enrolled in one of the Choice Plus medical plans administered by UnitedHealthcare (UHC) can also utilize:
- In and out-of-network benefit coverage (out-of-network services are subject to higher out-of-pocket expenses).
- Virtual care – UHC provides access to convenient virtual care. Connect 24/7/365 with quality board-certified doctors and pediatricians, as well as licensed counselors and psychiatrists.
- Health4Me Mobile App – provides instant access to health information, provider search capability, health plan ID card information and much more.
- Preventive care – free with in-network services; no copays, coinsurance or deductibles to meet for annual physicals and routine screenings – it is important to make sure your provider indicates the visit and services are for preventive care.
Fertility Solutions Program:
To support teammates and their covered spouses, treatment options covered through the Choice Plus medical plans may include (but are not limited to) bloodwork and testing, artificial insemination, IVF cycles and medically necessary cryopreservation. Please note: UHC support includes a clinical care team of experts and fertility Centers of Excellence (COE) to provide you and your family with the highest-quality care and service. If you live within 30 miles of a fertility COE, you will be required to receive fertility care through that COE. Click below for additional information.
- Fertility Solutions FAQs
- Click below to watch a Fertility Solutions Webinar
Well-being resources and services, at no-cost or low-cost through:
- 2nd.MD – Along with consulting 2nd.MD for the required consultations for spine, hip or knee surgery, teammates and family members can connect with board-certified, elite specialists through 2nd.MD about a new or existing diagnosis, treatment plan, possible other surgeries, medications or a chronic condition. Visit 2nd.md/bbinsurance or call 1-866-269-3534 for information.
- Omada Programs – Weight Loss and Diabetes Programs:
- Omada for Prevention – An online behavioral counseling support program designed to help at-risk individuals combat obesity-related chronic disease. Participants in the program learn how to make modest health changes that can lead to weight loss and reduced risk of type 2 diabetes and heart disease. Visit omadahealth.com/bbins to learn more.
- Important Note: Completion of the Omada program is a new requirement for weight loss medications as of 1/1/24. Review the following FAQs for additional information:
- Weight Loss Medications and Omada FAQs
- Omada for Diabetes – A personalized program that surrounds you with the tools and support you need to reach your wellness goals. Participants will be paired with a certified diabetes care and education specialist, have access to medications management support and to an online community. Visit omadahealth.com/bbins to get started.
- Omada for Prevention – An online behavioral counseling support program designed to help at-risk individuals combat obesity-related chronic disease. Participants in the program learn how to make modest health changes that can lead to weight loss and reduced risk of type 2 diabetes and heart disease. Visit omadahealth.com/bbins to learn more.
- Enhanced Substance Use Services – Platinum Preferred Facilities:
Teammates and dependents have the option of visiting any in-patient substance use facility available. However, selecting a Platinum Preferred facility, treatments are covered with no cost share when services are authorized. Click the Q&A below for additional information. - Substance Use Treatment Helpline – Access to a substance use recovery advocate that provides judgment-free support. Call the UHC Substance Use Treatment Helpline at 1-855-780-5955.
Clinical Management Programs:
- Genetic Testing, Radiology and Cardiology Prior Authorization through UHC for support in making the best decisions for health care quality and cost using evidence-based medicine if prior authorizations are required.
- 2nd.MD virtual medical consultations are required prior to a scheduled spine, hip or knee surgery. If a consultation is not completed, a $750 surcharge will be assessed to your claim. It is recommended to schedule a consult 30-days prior to a scheduled surgery. Call 1-866-269-3534 or visit 2nd.md/activate/step1/bbinsurance to initiate a consultation.
Prescription Drug Coverage:
- If enrolled in the Choice Plus HDHP, you will benefit from $0 copays for many preventive drugs, with no deductible to meet. This includes a variety of drugs for conditions such as asthma, cholesterol, depression, heart disease and high blood pressure.
- Before weight loss medications will be covered through either Choice Plus Plan, teammates and their covered dependents will be required to complete a healthy lifestyle management program with Omada®—a personalized virtual health program included in the UHC Choice Plus medical plans at no additional cost. Refer the Omada information under Well-Being Resources and Services above and review the following FAQs:
- Include step therapy to help you and your doctor choose a clinically effective, lower cost medicine as the first step in treating certain health conditions. Step therapy encourages individuals to first try less expensive, clinically appropriate options before “stepping up” to drugs that cost more. If you try (or have tried) a first line drug and it does not work for you, then you may receive coverage for a nonpreferred drug that your doctor prescribes.
- Prior authorization to help ensure our teammates are prescribed the most cost-effective and clinically appropriate medications for certain health conditions. This program makes sure you are getting a prescription that is suitable for the intended use and covered by your prescription plan.
Copay Assistance Program through PillarRx:
- Assists members in obtaining copay assistance from drug manufactures to reduce out-of-pocket expenses for eligible specialty medications.
Platinum Preferred Substance Use Coverage:
- When you or a loved one is facing the challenge of substance use, the last thing you want to worry about is the cost of receiving critical treatment. When you receive treatment at Platinum Preferred substance use facilities through UHC, services will be covered at 100% for teammates enrolled in our Choice Plus Copay and 100% after deductible for teammates enrolled in our Choice Plus HDHP.
Finding Providers
Medical – The National UHC Choice Plus Network; teammates residing in Massachusetts, New Hampshire and Maine will utilize the UHC Choice Plus with Harvard Pilgrim Network.
Labs – The UHC Choice Plus National Lab Network – Lab Corp. or Quest
To quickly find medical care within UHC Provider Networks follow the steps below:
To quickly find an Express Scripts Pharmacy:
Call the Brown & Brown Health Concierge Brown & Brown’s UHC helpline at 1-844-298-8929 with any questions.
Heading to your wellness exam?
At Brown & Brown Preventive Care is covered at 100% for all UHC medical plan participants and covers wellness exams, screenings, and immunizations.
A Preventive Care visit with your doctor is important as it may help uncover otherwise undetectable issues early, when health conditions are typically more treatable. To find more information or to get started with finding a doctor, click here.
Download the UnitedHealthcare Health4Me Mobile App. Sign-in with your UnitedHealthcare credentials to access Medical Care resources within your network.
Download the Express Scripts Mobile App. Sign-in with your Express Scripts credentials to access Prescription Drug Benefits resources within your network.
Frequently Asked Questions
Who can I call at UnitedHealthcare (UHC) for eligibility and claims questions?
- Brown & Brown Health Concierge: 1-844-298-8929
Who should I direct questions to regarding my prescription drug benefits?
- Express Scripts Patient Care Advocate: 1-800-745-3931
Who can I speak with regarding the Fertility Solutions Program?
- Call Fertility Solutions at 1-866-774-4626
Where can find information on the Fertility Solutions Program?
- Go to myuhc.phs.com/fertility – Use your HealthSafe ID to sign in
How can I find network providers?
- For Medical: Go to the UHC website at: myuhc.com
- For Prescription Drugs: Go to the Express Scripts Member Website as Follows:
- Pre-Member Website: express-scripts.com/brownbrowninc
- Member Website: express-scripts.com
How can I reach the Brown & Brown Team Resources Center?
- 1-866-505-0991 (Press 1) – Representatives available Monday-Friday from 8:00 a.m. to 6:00 p.m. ET, except holidays.
Hawaii Medical Plans
Hawaii Medical/Drug and Vision Plan Overviews
What are my plan options?
- Hawaii Medical Service Association (HMSA) CompMED / PPO with HMSA Vision Medical Plan
- Hawaii Medical Service Association (HMSA) HPH / HMO with HMSA Vision Medical Plan
- Hawaii Fully Insured Kaiser Permanente HMO With Kaiser Optical Medical Plan
The Group Number for both HMSA plans is 100116001.
The Group Number for the Kaiser plan is 10890.
Frequently Asked Questions
Hawaii Medical Service Association (HMSA) FAQs
Who can I call at Hawaii Medical Service Association (HMSA) for eligibility and claims questions?
- HMSA: 1-808-948-6111; or toll free at 1-800-776-4672
Who should I direct questions to regarding my prescription drug coverage?
- HMSA: 1-808-948-6111; or toll free at 1-800-776-4672
Who should I direct questions to regarding my vision coverage?
- HMSA: 1-808-948-6111; or toll free at 1-800-776-4672
How can I find network providers?
- Go to the HMSA website at https://www.hmsa.com
Kaiser Permanente FAQs
Who can I call at Kaiser Permanente for eligibility and claims questions?
- Kaiser: 1-800-966-5955
Who should I direct questions to regarding my prescription drug coverage?
- Kaiser: 1-800-966-5955
Who should I direct questions to regarding my vision coverage?
- Kaiser: 1-800-966-5955
How can I find network providers?
- Go to the Kaiser website at https://www.kpinhawaii.org/
How can I reach the Brown & Brown Team Resources Center?
- 1-866-505-0991 (Press 1)– Representatives available Monday-Friday from 8:00 a.m. to 6:00 p.m. ET, except holidays.
Proctor Loan Protector Medical Plans
Proctor Loan Protector Medical/Rx Plan Overviews
What are my plan options?
- Proctor Loan Protector BCBSM Simply Blue PPO Medical Plan
- Proctor Loan Protector BCBSM Simply Blue PPO/HSA Compatible Medical Plan
Frequently Asked Questions
Who can I call for eligibility, claims and prescription drug coverage?
- Blue Cross Blue Shield of Michigan: 1-888-288-2738
How can I find network providers?
- Already a member? Visit bcbsm.com and click on ‘Find a Doctor’ and log in to your online member account or click on ‘Search without logging in’
How can I reach the Brown & Brown Team Resources Center?
- 1-866-505-0991 (Press 1) – Representatives available Monday-Friday from 8:00 a.m. to 6:00 p.m. ET , except holidays.